Understanding the Science Behind Modern Dental Implant Success Rates
This post contains affiliate links. Click here to read my affiliate policy.
Last Updated on March 26, 2026
Dental implants have transformed restorative dentistry over the past three decades, evolving from an experimental procedure to the clinical gold standard for replacing missing teeth. With documented success rates consistently exceeding 95% at 10-year follow-up in well-selected patients, implants represent one of the most predictable interventions in modern medicine.
Yet the conversation around implants is often dominated by surface-level comparisons to dentures or bridges, obscuring the deeper science that explains why properly planned implant treatment delivers such durable results.
The American Academy of Implant Dentistry estimates that approximately 3 million Americans currently have dental implants, with 500,000 additional placements occurring annually. This growth reflects not just increasing patient awareness but continued refinement of materials, surgical techniques, and patient selection criteria that have made implants appropriate for a wider population than ever before.
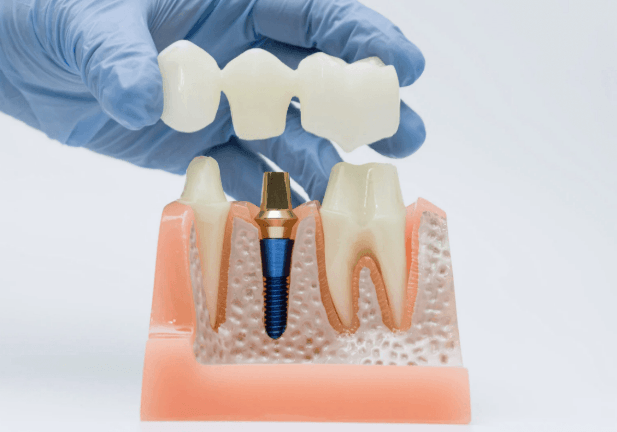
The Biology of Osseointegration
The fundamental mechanism that makes dental implants work is osseointegration, the direct structural and functional connection between living bone and the surface of a load-bearing implant. First described by Swedish orthopedic surgeon Per-Ingvar Branemark in the 1950s, osseointegration transformed implant dentistry from a theoretical concept to a clinical reality.
When a titanium implant is placed in the jawbone, a predictable biological sequence unfolds. Initial blood clot formation within hours creates the scaffold for cellular migration. Osteogenic cells from the surrounding bone begin colonizing the implant surface within days. Over the following months, woven bone is replaced by organized lamellar bone that provides the mechanical support necessary for long-term function.
The surface characteristics of modern implants are engineered to accelerate and enhance this process. Sandblasted and acid-etched surfaces, measured at the nanometer scale, increase the contact area available for bone attachment and stimulate osteoblast activity at the cellular level. These surface modifications have reduced the time required for adequate osseointegration from 6 months to as little as 6 to 8 weeks in optimal candidates, enabling faster restoration timelines without compromising long-term stability.
Zirconia implants, an alternative to titanium that has gained clinical traction in recent years, offer a metal-free option for patients with titanium sensitivities or aesthetic concerns in the anterior region. Long-term data comparable to titanium remains accumulating, but five-year outcomes from prospective studies are encouraging.
Patient Selection: Who Benefits Most from Implant Treatment
Not every patient presenting with a missing tooth is an equally strong candidate for implant therapy. Comprehensive evaluation of systemic health, local bone conditions, and oral hygiene habits determines who will achieve predictable long-term outcomes.
Bone volume and density at the proposed implant site are the primary anatomical considerations. Adequate bone must exist in three dimensions: width, height, and quality. Cone-beam computed tomography, which provides three-dimensional imaging of the jaw, allows precise measurement of available bone before treatment planning begins. When bone volume is insufficient, grafting procedures can create the necessary foundation, though they add time and complexity to the treatment sequence.
Systemic health factors that influence implant outcomes include:
- Controlled diabetes: Well-managed diabetes (HbA1c below 7%) does not significantly impair osseointegration. Poorly controlled diabetes increases infection risk and impairs healing.
- Smoking: Tobacco use reduces implant survival rates by approximately 20% due to impaired blood supply and immune function. The implant field’s consensus is that smoking cessation for 8 weeks before and 8 weeks after surgery significantly improves outcomes.
- Osteoporosis and bisphosphonate medications: Patients taking bone-modifying medications require specific risk stratification. Recent evidence suggests most bisphosphonate users can receive implants safely with appropriate precautions.
- Autoimmune conditions: Conditions requiring immunosuppressive medication increase infection risk and require individualized risk assessment.
Oral hygiene capability is equally important to physical health factors. Implants require the same diligent maintenance as natural teeth. Peri-implantitis, the implant equivalent of periodontitis, affects approximately 10% of implants over their lifetime and is the leading cause of late implant failure. Patients who demonstrate consistent brushing and flossing habits and who commit to regular professional maintenance visits achieve significantly better long-term outcomes.
The Restorative Dimension: Crowns, Bridges, and Full-Arch Solutions
The implant fixture itself is only one component of a complete implant restoration. The abutment that connects the implant to the visible crown, and the crown itself, each contribute to the long-term functional and aesthetic result.
Single-tooth implants, which replace an individual missing tooth with a standalone crown, are the most straightforward application. The crown is typically fabricated from lithium disilicate or zirconia, materials that match the appearance of natural enamel while providing durability sufficient for biting forces. Digital workflow technology, including intraoral scanning and CAD/CAM fabrication, has streamlined crown production while improving fit precision.
Implant-supported bridges replace multiple adjacent missing teeth using fewer implants than the number of teeth replaced. Three teeth can typically be restored on two implants, distributing occlusal forces across a larger implant footprint. This approach is biomechanically sound when the bridge design distributes forces appropriately and the opposing dentition does not create excessive lateral loading.
Full-arch rehabilitation, often marketed under names like “All-on-4” or “Teeth in a Day,” places four to six strategically positioned implants to support a complete arch of replacement teeth. This approach has transformed treatment options for patients with complete edentulism or terminal dentitions, providing fixed prostheses that eliminate the stability and psychological challenges of complete dentures. Patients seeking advanced dental implant solutions should discuss full-arch options with their provider if they are managing multiple failing teeth simultaneously, as planning the entire arch as a coordinated treatment can be more cost-effective than addressing teeth sequentially.
Maintenance and Long-Term Care
The 95%+ success rates cited in implant literature are achieved in patients who maintain their implants appropriately. Understanding what proper maintenance entails helps patients protect their investment.
Daily care requirements parallel natural tooth care: thorough brushing, interdental cleaning with floss or interdental brushes, and irrigation devices that access the gum-implant interface. Water flossers have shown particular effectiveness for disrupting bacterial biofilm around implants without the mechanical trauma risk associated with aggressive flossing techniques.
Professional maintenance visits at recommended intervals, typically every three to four months for the first year and every six months thereafter for patients without periodontal issues, allow early detection of peri-implant changes before they progress to peri-implantitis. These visits include professional cleaning with instruments designed specifically for implant surfaces, which differ from natural tooth surfaces in ways that standard scalers can damage.
Annual radiographic monitoring tracks bone levels over time. Stable bone is the primary objective indicator of implant health. Bone loss exceeding 1 to 2 millimeters during the first year or 0.2 millimeters annually thereafter signals a problem requiring investigation.
The Economic Perspective on Implant Investment
Dental implants carry a higher upfront cost than alternative replacements, typically ranging from $3,000 to $6,000 per tooth including the crown. This cost creates hesitation for patients who compare it to a bridge at $2,000 to $3,500 or a partial denture at $1,000 to $2,500.
The comparison changes substantially when lifetime costs are considered. Bridges require replacing the adjacent teeth to serve as abutments, potentially damaging healthy tooth structure. They typically need replacement every 10 to 15 years. Partial dentures affect adjacent teeth through clasping forces and commonly require rebasing and eventual replacement. Implants, maintained appropriately, routinely last 25 years or longer with only component-level repairs rather than full replacement.
For patients in their 40s or younger, the 30-year cost comparison typically favors implants by a significant margin, even before accounting for the superior functional and psychological outcomes that fixed implant restorations provide compared to removable alternatives.